Prostate Cancer
Make an Appointment
Our team of dedicated access representatives is here to help you make an appointment with the specialists that you need.
The prostate is a walnut-sized gland located just below your bladder. It produces most of the fluid found in semen. It also helps to expel semen during ejaculation.
Prostate cancer arises from cells in your prostate gland. It can spread to other parts of your body, most commonly to the lymph nodes and bones.
The specific causes of prostate cancer are not yet known. Researchers believe that genetic changes inside prostate cells may cause abnormal cell growth and eventually lead to cancer.
About 220,000 men are diagnosed with prostate cancer in the US each year. It is usually diagnosed in men over 50. Prostate cancer is the second most common cause of cancer-related deaths in men, behind lung cancer.
Screening for prostate cancer is key to catching the disease in its early stages, but guidelines for screening varies among expert organizations.
The American Cancer Society recommends that you talk to your doctor about prostate cancer screening when you turn 50, and the American Urological Association recommends to discuss screening at age 55.
The U.S. Preventive Services Task Force currently recommends to discuss prostate cancer screening between ages 55–69 but does not recommend routine screening over the age of 70.
You should talk to your doctor about whether prostate cancer screening is right for you.
If you’re at high risk—you’re African American or you have several family members who have had prostate cancer—you should talk to your doctor about prostate cancer screening when you’re 40 or 45.
Screening and Diagnosis
Rectal Exams and Blood Test
Prostate specific antigen, or PSA, is a blood test that looks for a protein made by the prostate and prostate cancer cells. When this test is used to screen healthy men between the ages of 55–69 years old, it can decrease prostate cancer death by about 20%. Your doctor will draw blood and pair it with a digital rectal exam for initial screening.
Novel Biomarkers
There are several new blood and urine tests that can help estimate the risk of having a prostate cancer. These tests are sometimes used to help make the decision about the need for further testing. You should ask your doctor if one of these tests would be helpful for you.
Needle Biopsy
The only way to determine if you have a prostate cancer is to perform a needle biopsy. This procedure is most commonly performed in the office by placing an ultrasound probe in the rectum, putting numbing medication around the prostate, and then inserting a small needle into the prostate.
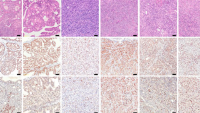
A pathologist examines the sampled cells under a microscope to see if cancer cells are present. If they are, they assign a Gleason Score, or Gleason Grade Group, to the tumor. This score is the grade of the cancer, is based on the appearance of the prostate cancer cells, and reflects aggressiveness.
In general, the higher the Gleason Score, or Gleason Grade Group, the more aggressive the cancer and the higher risk that the cancer will spread. Here’s a ranking of Gleason scores:
- Gleason Grade Group 1 (Gleason Score 6) : low grade and lower risk
- Gleason Grade Group 2 and 3 (Gleason Score 7): moderate risk
- Gleason Grade Group 4 and 5 (Gleason Score 8–10): high grade and aggressive
MRI
MRI has become increasingly used to evaluate men at risk for prostate cancer. Patients with an abnormal area in their prostate on MRI can have a targeted biopsy, which improves the accuracy of biopsy.
Symptoms
Because most prostate cancers are detected when they are very small as a result of PSA screening, most men with prostate cancer have no symptoms. However, patients with more advanced disease may have symptoms, including:
- A slowed urinary stream
- Difficulty starting or holding back urine
- Blood in the urine
- Pain in the hips and back (if cancer has spread to bones)
Some of these symptoms may be caused by a noncancerous medical condition called benign prostatic Hhyperplasia, or BPH.
Risk Factors
Prostate cancer is very common in the US. If you are diagnosed with prostate cancer, it is not your fault. There are several known risk factors:
- Age. Age is the biggest risk factor for prostate cancer. More than 60% of prostate cancers are detected in men over 65.
- Race. Prostate cancer is more common in men of African descent.
- PSA. While we use PSA to determine your current risk of prostate cancer and determine the need for additional testing, your PSA level is also predictive of your future risk of prostate cancer. Young men with a very low PSA are unlikely to be diagnosed with an aggressive prostate cancer.
- Family history. Prostate cancer tends to run in families, suggesting a genetic connection. If your father or brother had prostate cancer, you’re twice as likely to develop it too.
- Genetic predisposition. Some patients with a hereditary genetic mutation, a change in a gene inherited from their parents, may be at increased risk for prostate cancer. At this time, there are several genetic mutations that have been associated with prostate cancer, including BRCA and Lynch syndrome. If you have a genetic mutation that increases your risk of a cancer, you should discuss prostate cancer screening with your doctor.
Related
Prostate Cancer Patient Guides & Resources from the Dept of Urology